BEFORE introduction please use high CPC keywords for Google AdSense such as dermatology treatment tips eczema relief strategies skin barrier repair guide occupational dermatitis prevention premium medical content atopic dermatitis management high‑earnings health article ad therapy optimization functional skin health content AdSense health monetization
Scientists and dermatology experts are shedding new light on hand dermatitis—also known as hand eczema—unpacking its symptoms, causes, and targeted healing strategies that go far beyond a skin discomfort adventure. This deep dive serves as a functional skin health content resource and a premium medical content article that uses eczema relief strategies and skin barrier repair guide insights, designed for high‑earnings health article performance and optimized AdSense health monetization.
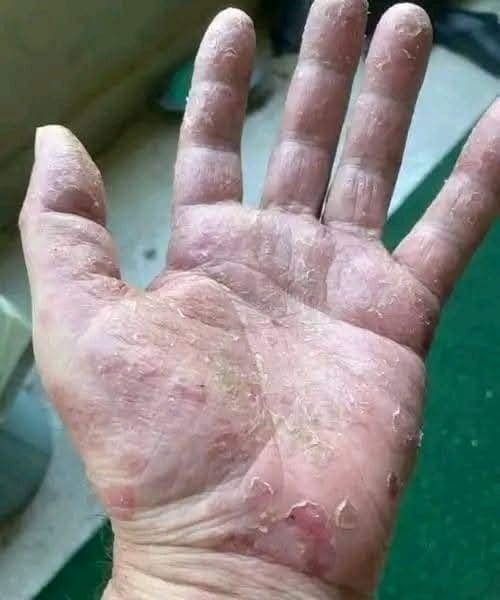
Hand dermatitis can be mild to severe and is often mistaken for dry skin until its relentless symptoms become unmistakable. Defined by red, itchy, dry, cracking, or blistering palms and fingers, it may even bleed, crust, or pain deeply in chronic cases. Some people experience thickened, leathery skin or leathery patches that evolve over time, signaling a deeper barrier dysfunction rather than temporary drought. Healthcare professionals and authoritative sources underscore that effective management must target both inflammation and skin barrier reinforcement. Diagnosis typically starts with a clinical evaluation of the hands’ physical condition, a review of history, and, if needed, patch testing. In certain complex cases, a skin biopsy can clarify the underlying type of hand eczema .
Causes and triggers of hand dermatitis are multifactorial and warrant a detailed understanding to guide both individuals and clinicians toward smarter prevention. Irritant contact dermatitis arises when daily exposure to harsh agents—such as cleaning chemicals, detergents, solvents, prolonged or repeated water contact, friction, or temperature extremes—break down the skin’s natural oils and compromise barrier integrity . Allergic contact dermatitis, on the other hand, stems from immune reactions to specific allergens like nickel in jewelry, latex in gloves, or common fragrances and preservatives in soaps, lotions, and detergents. Plants and industrial agents may also trigger responses in sensitized individuals . Occupational exposures—such as frequent hand washing in healthcare, chemical and construction work—dramatically amplify the risk of hand eczema .
Symptoms typically begin with dry, chapped skin and escalate to red or dark brown patches, inflamed scaly areas, burning or itching sensations, and visible vesicles or blisters. Cracking, bleeding, crusting, pus, and severe pain with chronic thickening are alarm signals that require medical attention . These symptoms often mirror other dermatological issues like psoriasis or fungal infections, making precise diagnosis essential.
A multi‑layered management plan for hand dermatitis is critical to provide eczema relief strategies, with combined home care, lifestyle shifts, and medical interventions that repair the barrier and reduce flare‑ups. At home, daily moisturizing with fragrance‑free emollients and ointments rich in glycerin, ceramides, shea butter, petrolatum, or mineral oil is foundational—ideally applied immediately after hand washing and frequently throughout the day . Lukewarm water should be used to wash hands—hot water strips away vital oils—while gentle patting to dry (not rubbing) preserves hydration . Use mild, fragrance‑free cleansers and soaps; select products labeled fragrance‑free (not merely “unscented”) to minimize irritants . Protective gloves—nitrile or vinyl with a cotton liner—should be worn when handling water, detergents, or harsh chemicals; cotton-lined gloves reduce sweat‑related irritation .
For soothing flares, home remedies like overnight application of petroleum jelly under cotton gloves support barrier repair. Lukewarm oatmeal baths (using colloidal oatmeal) can calm inflammation. Aloe vera helps soothe and hydrate, while stress reduction and a balanced diet rich in omega‑3 fatty acids and water support skin resilience . Humidifiers maintain ambient moisture to prevent air‑driven skin dryness .
When symptoms persist or moderate to severe inflammation occurs, pursuing medical treatments under dermatologist guidance is wise. Topical corticosteroids are the mainstay for flare management, yet need caution due to risks like skin thinning, especially with long-term use on thick skin areas like palms . Non‑steroidal topical calcineurin inhibitors like tacrolimus and pimecrolimus offer alternatives for sensitive areas, although their absorption in palmar skin may differ . Phototherapy under medical supervision is viable for chronic or refractory cases .
Systemic therapies—reserved for severe, unresponsive cases—include oral corticosteroids, retinoids like alitretinoin (approved in select regions), immunosuppressants such as cyclosporine and methotrexate, and mycophenolate mofetil—with varying efficacy and potential side effects . Rapidly emerging biologic and small‑molecule therapies are expanding the therapeutic toolkit: dupilumab (IL‑4/IL‑13 inhibitor) shows promising hand eczema improvement in AD patients. JAK inhibitors like delgocitinib (topical pan‑JAK) and oral gusacitinib are in trials with encouraging results for reducing hand lesion severity .
Effectively managing hand dermatitis requires a layered approach combining consistent skin care habits, barrier repair strategies, protective measures, stress control, dietary mindfulness, and professional medical treatments when needed—a comprehensive plan aligned with long‑term AD therapy optimization and functional skin health content goals.
Below is an extended breakdown of each domain:
For complete cooking times, go to the next page or click the Open button (>), and don't forget to SHARE with your Facebook friends.